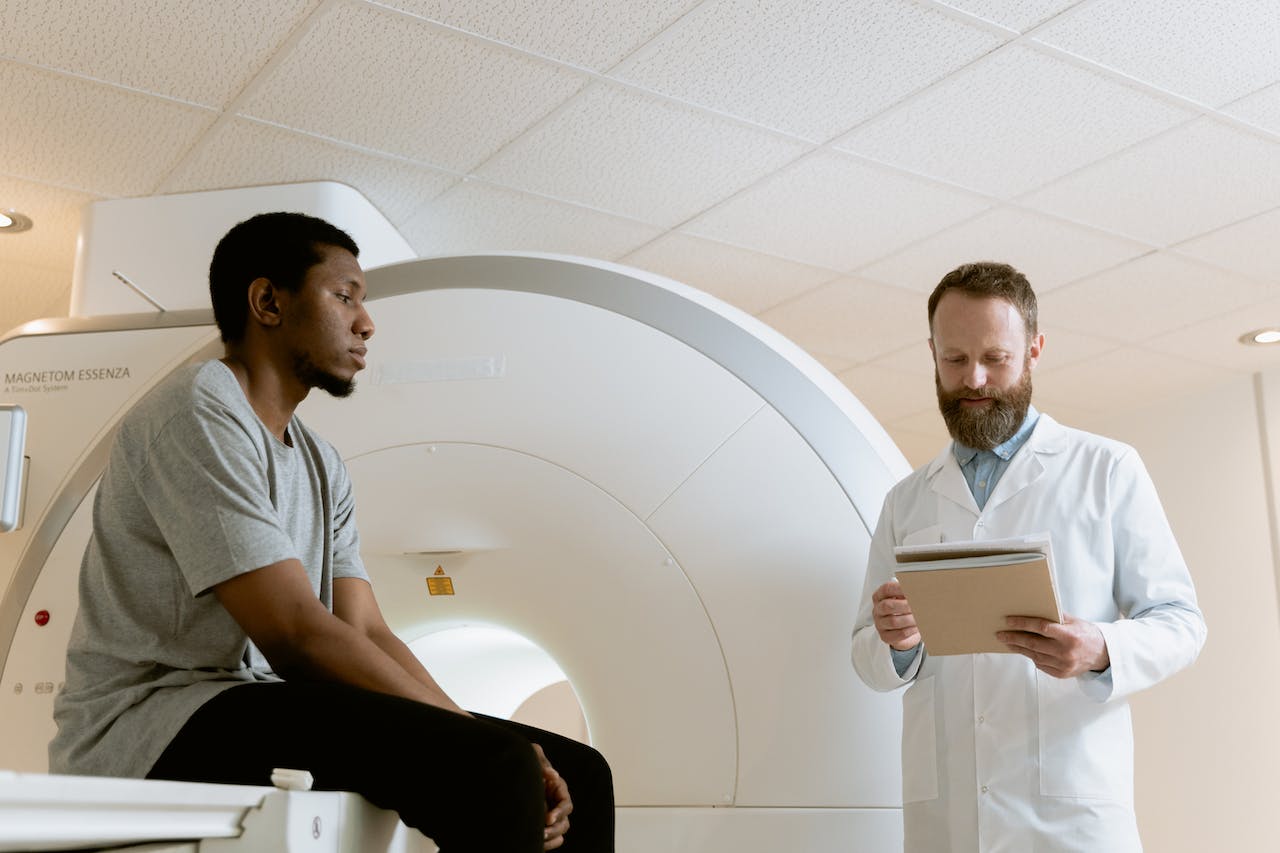
Opioid Use Disorder and Chronic Pain
Opioid use disorder (OUD) and chronic pain are complex issues that often occur together, posing significant challenges for patients and healthcare providers alike. Examining the reasons behind opioid misuse, exploring alternative medications, and considering the role of medication-assisted treatment (MAT) in pain management are all parts of making sure a person gets the treatment they need. People from all walks of life have been diagnosed with a substance use disorder. OUD is no different.
Why Do People Misuse Opioids?
Opioids are potent analgesics commonly prescribed for managing moderate to severe pain. Even when used as prescribed, they can lead to tolerance and dependence. People are more likely to misuse the drug the longer they are on it; most opioids are meant to be used by people in moderate to severe pain, such as from an operation or an acute injury.
Underlying mental health issues, social and environmental influences, and genetic predisposition may also contribute to opioid use disorder. People who have experienced trauma or abuse are more likely to use opioids.
Alternatives to Opioids for Pain
Non-opioid analgesics like acetaminophen and nonsteroidal anti-inflammatory drugs (NSAIDs) are effective for certain types of pain. Antidepressants (tricyclic antidepressants and serotonin-norepinephrine reuptake inhibitors), such as Amitriptyline, can often help with nerve pain. Neurological drugs like gabapentin can also help with some types of pain. Some people who live with debilitating conditions find that physical therapy can teach them to move without pain and build muscles to prevent injury.
Medication-Assisted Treatment (MAT) and Chronic Pain Management
MAT, encompassing opioid agonist therapy (OAT) with methadone or buprenorphine and opioid receptor antagonist naltrexone, can help individuals with OUD manage cravings and withdrawal symptoms. An integrated MAT approach addresses both opioid use disorder and chronic pain simultaneously, offering a more holistic care strategy.
Support groups, including counseling, support groups, and mental health interventions, are essential in addressing the psychological and social aspects of chronic pain. People with opioid use disorder thrive when given the opportunity to get sober and learn about their disorder. Patient education, focusing on the risks and benefits of medications, coping strategies, and the nature of chronic pain, empowers individuals to actively participate in their treatment.
Living with chronic pain can be a daunting challenge, and for many people, opioids have been a common solution. As the opioid crisis continues, there is a growing awareness of the need for alternatives. Advocating for these alternatives can be a powerful way for chronic pain patients to actively shape their treatment plans and promote safer, more effective pain management strategies.
Advocating for Chronic Pain Alternatives to Opioids
Opioids may provide relief initially but can lead to tolerance, dependence, and other adverse effects. Understanding the broader landscape of pain management opens the door to exploring alternative approaches. If you live with chronic pain and addiction, it’s a good idea to become an advocate for yourself. Much of chronic pain treatment can benefit people, but you need to know about the various solutions available.
Research and stay informed about non-opioid alternatives that align with your specific pain condition. Non-opioid analgesics like acetaminophen and NSAIDs, medications such as antidepressants and anticonvulsants, and various physical and behavioral therapies are viable options. Many people use mindfulness to help with pain flares and spasms, while people who live with headache disorders often have options like steroidal or Botox headache injections. Knowledge empowers you to engage in meaningful discussions with your healthcare provider.
You can work collaboratively with your healthcare provider to develop a personalized pain management plan that incorporates non-opioid interventions. This plan should outline the various strategies you will explore, the expected outcomes, and a timeline for reassessment. Having a clear plan in place can provide a sense of direction and purpose. It can prevent you from giving up. Discuss the potential benefits and risks of each proposed treatment and make decisions together that align with your goals and values.
Joining patient advocacy groups focused on chronic pain can provide a supportive community and valuable resources. These groups often share information about alternative treatments, advocate for policy changes, and offer guidance on navigating the healthcare system.
Consider sharing your pain management journey, including successes and challenges, with others in recovery. Personal narratives can be powerful tools for raising awareness about staying sober as a chronic pain patient. Whether through social media or local support groups, your story may inspire others and contribute to helping others with pain issues learn to cope while remaining clean and sober.
If you are in need of help, please call us at: 910-295-7246 or message us.
Categories
health Treatment
